In 1944, Don Gardner wrote the famous song with lyrics that included “All I want for Christmas is my two front teeth”. Little did he know that over 72 years later, we can make this wish become a reality in one day. It is interesting to see how many of our patients are trying to restore their smiles and function before the holidays. With the current implant design features which include roughened surfaces, tapered implant bodies, and aggressive thread patterns, we have been able to place implant fixtures into extraction sockets and then attach temporary abutments and crowns with great predictability and success. Fully edentulous arches can be restored on just four implant fixtures. These procedures are incredibly gratifying for both the patients and the practitioners. Although we have been placing implants in our practice for over 30 years, the excitement continues as the technology evolves! Happy Holidays!
PERIODONTAL ASSOCIATES
photo credit: Zazzle
Better oral hygiene and regular dental visits may play a role in slowing cognitive decline as people age, although evidence is not definitive enough to suggest that one causes the other. The findings, published in the Journal of the American Geriatrics Society, come from the first systematic review of studies focused on oral health and cognition–two important areas of research as the older adult population continues to grow, with some 36% of people over age 70 already living with cognitive impairments.
Researchers have questioned whether an association exists between oral health and cognitive status for older adults. “Clinical evidence suggests that the frequency of oral health problems increases significantly in cognitively impaired older people, particularly those with dementia,” said Bei Wu, PhD, of Duke University’s School of Nursing in Durham, NC. “In addition, many of the factors associated with poor oral health–such as poor nutrition and systemic diseases like diabetes and cardiovascular disease–are also associated with poor cognitive function.”
To look for a link between oral health and cognitive status, Dr. Wu and her colleagues analyzed relevant cross-sectional (data collected at one specific point in time) and longitudinal (data collected over an extended period of time) studies published between 1993 and 2013.
Some studies found that oral health measures such as the number of teeth, the number of cavities, and the presence of periodontal disease (also known as “gum disease”) were associated with an increased risk of cognitive decline or dementia, while others studies were unable to confirm any association. Researchers were also quick to note that findings based on the number of teeth or cavities are conflicting, and limited studies suggest that periodontal conditions such as gingivitis are associated with poorer cognitive status or cognitive decline.
“There is not enough evidence to date to conclude that a causal association exists between cognitive function and oral health,” said Dr. Wu. “For future research, we recommend that investigators gather data from larger and more population representative samples, use standard cognitive assessments and oral health measures, and use more sophisticated data analyses.”
Journal Reference:
- Bei Wu, Gerda G. Fillenbaum, Brenda L. Plassman, and Liang Guo.Association Between Oral Health and Cognitive Status: A Systematic Review. Journal of the American Geriatrics Society, April 1, 2016 DOI:10.1111/jgs.14036
Source: Science Daily
Wiley. “Is there a link between oral health and the rate of cognitive decline?.” ScienceDaily. ScienceDaily, 1 April 2016. <www.sciencedaily.com/releases/2016/04/160401073706.htm>;.
Densah bur Versahtility allows one to take on many different implant situations without compromising the alveolus and the implant stability. Less removal of bone via the osteotomy procedure and preservation of the alveolar anatomy by osseodensification creates an optimum implant site. One can also lift the sinus floor by autognenous elevation by utilizing the Densah burs to create a site for optimum length of implants placed. Log on to the site to view the information and videos on the use of the bur system- http://versah.com
Advantages of the system:
Stable yet removable solution that offers the comfort of a fixed prosthesis
Easy to clean
Optimal chewing and function
Desirable phonetics and esthetics
A cost effective solution
Another great All-on-4 dental implant case with computer guided surgery in partnership with Ira and Brandon Dickerman of Dickerman Dental Prosthetics! The patient was scanned in a Carestream CS 9300 CBCT scanner while wearing a surgical/diagnostic guide with radiopaque teeth. With that information, the virtual implants and other components are located within the prosthesis and bone during an online treatment planning conference session with the doctor and lab technician. The locking pins are also located which will stabilize the guide on the arch during surgery.
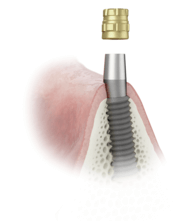
This case was set up for the use of Nobel Biocare NobelReplace Conical Connection implants which provide maximum stability due to the tapered body design, and crestal bone preservation due to the horizontal “platform shift” of the restorative table. Of course, the proprietary NobelBiocare surgical kit must be used for the implants in this particular case. However, any dental implant that is designed for guided surgery may be used, per the choice of the surgeon, as long as that manufacturer’s guided surgery kit is utilized.
The surgery typically involves minimal discomfort for the patient and can be completed in significantly less time than conventional implant surgery.
These cases are cost-effective, durable, and esthetic, which vastly improves the quality of our patients’ lives.
My partner, Giovanni Castellucci, and I have been placing dental implants in our periodontal practice for over 27 years. In the early days, the Branemark “hybrid” prosthesis was the standard of care for restoration of fully edentulous patients with five or six implant fixtures. We followed the traditional two-stage protocol and our patients enjoyed tremendously successful outcomes which have improved their quality of life. However, as time progressed, the hybrid prosthesis became less popular as more conventional PFM fixed restorations were fabricated on custom abutments.
In recent years, we have seen a resurgence of the use of the hybrid prosthesis with the “All-On-4” Immediate Dental Implant (Teeth in a Day) protocol. Now, we successfully restore fully edentulous arches on four implant fixtures on the same day that the hopeless teeth are removed, oftentimes without the need for bone grafts. Our patients are thrilled with the results, and the functional and esthetic benefits are instant.
When speaking with many of our restorative colleagues in Boston, Newton, Framingham, and the Metrowest communities, I occasionally hear them say “my practice doesn’t have edentulous patients“, or “we don’t make dentures”. This would imply that the demographic profile of these practices does not include a major component of the general population. Yet, we know that millions (if not billions) of dollars are spent annually on denture adhesives, and that the national dental clinics that focus on denture fabrication are thriving. And, let us not forget that many people with hopeless teeth due to severe gum disease or decay oftentimes avoid treatment because of fear of having to wear a complete removable denture. The “All-On-4” treatment is the perfect solution for these patients as they can have their natural teeth replaced by non-removable, fixed implant-supported teeth on the same day in one dental appointment.
In our practice, we see “All-On-4” patients from all communities, even the most affluent. After all, dental and periodontal diseases do not discern one community from another. With this in mind, we urge all clinicians to “open their eyes” to the benefits of immediate dental implant restorations as another tool to help enhance the lives of our patients.
Have any of you had similar experiences? Please share them with the community.
Cary Feuerman, DMD
PERIODONTAL ASSOCIATES
photo credit:

I came across the following information written by Julie Revelant which is timeless and always useful for pregnant women.
You’ve cut down on coffee, nixed sushi, and exercise most days, but what you may not realize is that oral health is just as important when you’re pregnant.
Dental problems during pregnancy are quite common, with approximately 40 percent of women who have gingivitis, cavities, and periodontitis, according to a recent report by the American College of Obstetricians and Gynecologists (ACOG). And left untreated, many conditions can be harmful to you and your baby.
Here, find out why dental problems are more common during pregnancy, if you’re at risk, and what you can do about it.
Pregnancy gingivitis and more.
One of the most common dental conditions is pregnancy gingivitis, which can cause red, tender, and swollen gums that bleed easily. Some women may even develop a benign tumor in their mouths, which can be removed or will resolve itself after giving birth, according to Dr. Joseph Banker, founder of Creative Dental Care in Westfield, NJ.
Pregnancy gingivitis occurs because the increase in the hormone progesterone during pregnancy causes an exaggerated response to the plaque that’s already in your mouth. “The reaction to those toxins and those poisons from the plaque build-up is increased,” according to Dr. Amanda Seay, Orbit for Kids gum spokesperson.
And even if you’re diligent about brushing and flossing, pregnancy gingivitis can still be a problem. If left untreated, it can lead to periodontal disease, which studies show increases your risk for having a preterm and low birth weight baby.
Plus, if you have a history of periodontal disease, you’re more likely to have dental problems during pregnancy as well.
If you’re pregnant or planning to become pregnant, here’s what you can do to prevent dental problems.
Brush and floss.
Brushing after every meal and flossing at least once a day are the best ways to keep your teeth and gums healthy. Go one step further with an alcohol-free rinse and a tongue scraper which both remove bacteria, Banker said.
Go to the dentist.
According to the same ACOG report, between 2007 and 2009, 35 percent of women had not seen a dentist within the past year and more than half had not seen one during pregnancy either. Experts agree that if you’re trying to become pregnant or undergoing infertility treatment, getting your oral health in check beforehand is a no-brainer.
Get cleanings every 6 months or more.
Research shows there is no risk having routine dental care during pregnancy, and dental cleanings are your best line of defense. Every 6 months is ideal, but your dentist may recommend more frequent cleanings especially if you have a history of gingivitis or periodontal disease.
Eat right.
It can be a challenge to eat healthy when you’re dealing with morning sickness, but trying to avoid sticky foods and eating course, fiber-filled fruits and vegetables, nuts, and cheese can help. If you drink soda or coffee with sugar, have a cup but don’t sip on it all day, Banker said.
Chew gum and drink water.
“Saliva is the greatest natural defense mechanism that we have,” Seay said. If it’s been hours between brushing, chewing a sugar free gum with xylitol can increase the salivary flow which washes away food debris, neutralizes plaque acids, and keeps bacteria at bay. After a meal, drinking a glass of water can help too.
Treat infections.
“If there’s an emergency, you have to deal with it,” Banker said. And the risk of infection from an untreated dental problem, like an abscess, poses a greater risk to you and your baby than the dental procedure itself. In fact, a dental infection can cause pre-eclampsia, pre-term birth, developmental delays—even miscarriage.
New ACOG recommendations say dental x-rays are safe since most dentists now use digital x-rays, which have 10 to 20 percent of the previous amount of radiation. Plus, the abdominal shield and thyroid collar, “blocks out almost—if not all—the radiation that would even get near the developing baby,” Banker said.
Blog written by Juiie Revelant for Fox News.com. Julie Revelant is a freelance writer and copywriter specializing in parenting, health, healthcare, nutrition, food and women’s issues. She’s also a mom of two. Learn more about Julie at revelantwriting.com
Alligators may help scientists learn how to stimulate tooth regeneration in people, according to new research led by the Keck School of Medicine of USC.
For the first time, a global team of researchers led by USC Professor Cheng-Ming Chuong has uncovered unique cellular and molecular mechanisms behind tooth renewal in American alligators. Their study appeared in Proceedings of the National Academy of Sciences, the official journal of the National Academy of Sciences.
“Humans naturally only have two sets of teeth — baby teeth and adult teeth,” Chuong said. “Ultimately, we want to identify stem cells that can be used as a resource to stimulate tooth renewal in adult humans who have lost teeth. But to do that, we must first understand how they renew in other animals and why they stop in people.”
Whereas most vertebrates can replace teeth throughout their lives, human teeth are naturally replaced only once, despite the lingering presence of a band of epithelial tissue called the dental lamina, which is crucial to tooth development. Because alligators have well-organized teeth with similar form and structure as mammalian teeth and are capable of lifelong tooth renewal, the authors reasoned that they might serve as models for mammalian tooth replacement.
“Alligator teeth are implanted in sockets of the dental bone, like human teeth,” said Ping Wu, assistant professor of pathology at the Keck School and first author of the study. “They have 80 teeth, each of which can be replaced up to 50 times over their lifetime, making them the ideal model for comparison to human teeth.”
Using microscopic imaging techniques, the researchers found that each alligator tooth is a complex unit of three components — a functional tooth, a replacement tooth and the dental lamina — in different developmental stages. The tooth units are structured to enable a smooth transition from dislodgement of the functional, mature tooth to replacement with the new tooth. Identifying three developmental phases for each tooth unit, the researchers concluded that the alligator dental laminae contain what appear to be stem cells from which new replacement teeth develop.
“Stem cells divide more slowly than other cells,” said co-author Randall Widelitz, associate professor of pathology at the Keck School. “The cells in the alligator’s dental lamina behaved like we would expect stem cells to behave. In the future, we hope to isolate those cells from the dental lamina to see whether we can use them to regenerate teeth in the lab.”
The researchers also intend to learn what molecular networks are involved in repetitive renewal and hope to apply the principles to regenerative medicine in the future.
The authors also reported novel cellular mechanisms by which the tooth unit develops in the embryo and molecular signaling that speeds growth of replacement teeth when functional teeth are lost prematurely.
Co-authors included colleagues from the Louisiana Department of Wildlife and Fisheries, University of Georgia, National Cheng Kung University, National Taiwan University and Xiangya Hospital in China.
The research was supported by the National Institute of Arthritis and Musculoskeletal and Skin Diseases (grant numbers 5R01AR042177-19, 5R01AR060306-03 and 2R01AR047364-11A1).
SOURCE: University of Southern California
Tobacco and alcohol use are the most well-known risk factors for oral and pharyngeal (throat) cancer. Other important factors include diet and a strain of human papilloma virus (HPV 16), which is sexually transmitted. Genetic susceptibility can also play a role; most human diseases result from the interaction of your genes and environmental factors that may be chemical, physical, nutritional, or infectious, for example. But while we cannot control our genetic makeup, there are a number of lifestyle choices we can make in order to decrease the risk for oral cancer. Avoidance of tobacco, moderation in alcohol intake, avoiding risky sexual behavior, and eating a plant-based, whole-food diet can reduce the risk not only for oral cancer, but also for other common cancers, as well as chronic diseases such as heart disease.
The Link Between Diet And Cancer
A strong body of research over the past 50 years has established a link between diet and cancer, though the mechanisms for this connection are only partially understood. The process of carcinogenesis (“carcino” – cancer; “genesis” – origination) may be initiated by damage to DNA, the genetic material that contains crucial instructions that define each cell in the body and what it does. So how does cellular DNA become damaged? We are constantly exposed to environmental factors that can damage our DNA. The balance of harmful and beneficial exposures, and how they interact will determine if DNA will be damaged.
For example, a class of chemicals known as nitrosamines has been shown to be carcinogenic. Nitrosamines can be formed when nitrites used to preserve meat, such as bacon and ham, are ingested. Nitrosamines are also found in beer, fish and fish byproducts, cheese products, and other foods preserved with nitrite pickling salt.
DNA can also be damaged when it is exposed to “free radicals,” unstable molecules that are produced constantly during normal cellular function. Antioxidants protect the cells from damage caused by these free radicals. Your body therefore needs a good supply of antioxidants, and this is why dietary antioxidants are so important.
Phytonutrients (nutrients derived from plant foods) such as vitamins C and E have antioxidant properties and may prevent DNA damage by reducing exposure to free oxygen radicals. Adoption of a diet rich in plant foods, particularly fruits and vegetables, has been shown to increase the intake of these protective dietary factors. They include antioxidant vitamins; carotenoids (antioxidant compounds that give red and orange fruits and vegetables their color); lycopene (a carotenoid that makes tomatoes red); and fiber. At the same time, eating more plant foods will decrease your intake of pathogenic (disease-causing) dietary factors, including total fat, saturated fat, animal protein and nitrates.
It’s important to note that dietary supplements, including vitamins and minerals, have not been shown to be effective substitutes for a diet high in fruits and vegetables. The protective benefits of antioxidants are most likely to come from ingesting them naturally in foods, not in pill form.
Investigators in epidemiologic studies have consistently found that a high intake of fruits vegetables reduce the risk for oral and throat cancer, as well as cancer occurring at other sites, including the esophagus (gullet), breast, prostate, lung, bladder and colon. According to the American Cancer Society, “evidence suggests that a third of the more than 500,000 cancer deaths that occur in the United States each year can be attributed to poor diet and physical inactivity.”
Other Important Steps Toward Prevention
As mentioned earlier, moderating alcohol intake and tobacco cessation are very positive steps you can take toward cancer prevention that your dentist or doctor can help you with. Understanding the risk of sexual transmission of HPV and reducing the likelihood of exposure to the virus is another important step. A whole-foods, plant-based diet, exercise and regular checkups with your dentist and doctor are important for maintaining good oral and general health.
Source: Dear Doctor – Dentistry & Oral Health
One out of every two American adults aged 30 and over has periodontal disease, according to recent findings from the Centers for Disease Control and Prevention (CDC). A study titled estimates that 47.2 percent, or 64.7 million American adults, have mild, moderate or severe periodontitis, the more advanced form of periodontal disease. In adults over age 65, prevalence rates increase to 70.1 percent. This study is published in the Journal of Dental Research, the official publication of the International and American Associations for Dental Research.
Periodontal disease is a chronic inflammatory disease that affects the gum tissue and bone supporting the teeth, according to the American Academy of Periodontology (AAP). If left untreated, periodontal disease can lead to tooth loss. Research has also shown that periodontal disease is associated with other chronic inflammatory diseases, such as diabetes and cardiovascular disease. The AAP has worked closely with CDC since 2003 on periodontal disease surveillance.
The findings are based on data collected as part of CDC’s 2009-2010 National Health and Nutrition Examination Survey (NHANES), designed to assess the health and nutritional status of adults and children in the United States. The 2009-2010 NHANES included for the first time a full-mouth periodontal examination to assess for mild, moderate, or severe periodontitis, making it the most comprehensive survey of periodontal health ever conducted in the U.S. Researchers measured periodontitis because it is the most destructive form of periodontal disease. Gingivitis, the earliest stage of periodontal disease, was not assessed.
“This is the most accurate picture of periodontal disease in the U.S. adult population we have ever had,” said Dr. Pamela McCain President of the American Academy of Periodontology and a practicing periodontist in Aurora, Colorado. “For the first time, we now have a precise measure of the prevalence of periodontal disease, and can better understand the true severity and extent of periodontal disease in our country. The AAP values its collaboration with CDC to better understand the burden of periodontal disease in Americans.”
The findings also indicate disparities among certain segments of the U.S. population. Periodontal disease is higher in men than women (56.4 percent vs. 38.4 percent) and is highest in Mexican-Americans (66.7 percent) compared to other races. Other segments with high prevalence rates include current smokers (64.2 percent); those living below the federal poverty level (65.4 percent); and those with less than a high school education (66.9 percent).
As we know, the best treatment is prevention. Patients should contact their local dentist or periodontist for a comprehensive examination. It is never too early as the signs of disease often don’t present themselves until the disease has become more advanced.
SOURCE: American Academy of Periodontology
PHOTO CREDIT: AAP