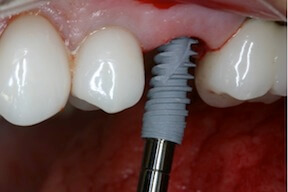
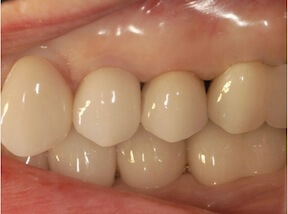
Imagine that you are a dentist who wants to consult an endodontist some distance away about a problem a patient is having. You need to send her the patient’s x-rays in a fast and secure manner. Today, you may have trouble transmitting the images digitally if you and the other dentist use different systems. To make the transfer seamless, the systems must be interoperable. That’s where the ADA is contributing to a solution.
The ADA is working to ensure that dental offices can exchange diagnostic digital images and patient data securely with other healthcare entities, no matter what system they use. The ADA’s Standards Committee on Dental Informatics (SCDI) serves as the sponsor of the Dental Domain under the independent standards group known as Integrating the Healthcare Enterprise (IHE). SCDI is leading the team of experts that is developing the standards and testing the software that will make that goal a reality.
“We are responding to ADA members who have told us, ‘I can’t exchange my dental images with the specialist down the street because we have different software and computer systems’,” said Dr. Kirt Simmons, Dental Domain co-chair for IHE. “This collaboration [between the ADA and IHE] is working on solutions that will help dentists to select interoperable systems allowing for the secure and private exchange of images while maintaining HIPAA compliance.”
By 2014, SCDI will sponsor the first IHE Connectathon, an annual event where vendors of dental systems will test their systems for conformance to the new interoperability standards, as verified by independent judges. An interoperability demonstration is also planned for the 2014 ADA Annual Session.
Additional Resources:
Interoperability of digital dental imaging files is made possible through DICOM, a standardized file format that makes possible the export and import of digital medical images and data between systems in a secure manner. More information on DICOM and interoperability of digital dental imaging systems can be found in ADA Technical Report No. 1057, Guidelines for Digital Imaging Systems and Interoperability in Today’s Dental Practice available through the ADA Catalog.
HIPAA compliance is a major factor when considering exchange of digital images. The ADA makes available numerous information sources on HIPAA at ADA.org/HIPAA.
Source: American Dental Association
The ADA Council on Scientific Affairs has issued new guidance on the use of cone-beam computed tomography (CBCT) in dentistry. Their findings appear in an advisory statement in the August issue of the Journal of the American Dental Association.
The Council concluded that clinicians should prescribe CBCT imaging only when they expect that the diagnostic yield will benefit patient care, enhance patient safety or improve clinical outcomes significantly.
The advisory statement discusses:
- Principles for the safe and appropriate use of CBCT imaging procedures, including sound clinical justification, optimal radiation protection and using the smallest field of view necessary for diagnostic purposes
- Precautions for the safety of the patient and the dental team
- Appropriate education and training for CBCT imaging and evaluation
Read the entire advisory statement in the August issue of JADA.
The U.S. Food and Drug Administration (FDA) has also posted an informational webpage on dental cone-beam computed tomography. The FDA is promoting the safe use of CBCT in dental and maxillofacial imaging, particularly in the pediatric population. Recommendations are provided for parents, patients and health care providers to help reduce unnecessary radiation exposure from CBCT.
SOURCE: American Dental Association
The FDA has reissued a warning about the use of benzocaine gels or liquids to relieve teething pain for children under two years old. Parents should not use over-the-counter medications containing benzocaine for children under two years old because they are at particular risk for the rare but serious disease of methemoglobinemia, a disorder in which the amount of oxygen carried through the blood stream is greatly reduced. The most severe cases can result in death. Adults with heart disease or breathing problems and smokers are also at greater risk for the disease.
Concern is fueled by the serious potential outcomes and the difficulty parents may have recognizing the signs and symptoms of methemoglobinemia when using these products at home. The symptoms may not always be evident or attributed to the condition. They include pale skin, lips and nail beds; shortness of breath; and fatigue.
Instead of using the benzocaine teething products, the FDA advises to follow these recommendations from the American Academy of Pediatrics’ for treating teething pain:
- Give the child a teething ring chilled in the refrigerator.
- Gently rub or massage the child’s gums with your finger to relieve the symptoms of teething.
For more information, visit http://go.usa.gov/dY1.
Source and Photo Credit: American Dental Association
Another recent study confirms why women should keep those toothbrushes and dental floss handy! A comprehensive review of women’s health studies by Charlene Krejci, associate clinical professor at the Case Western Reserve University School of Dental Medicine, has shown a link between women’s health issues and gum disease.
Across the ages, hormonal changes take place during puberty, menstruation, pregnancy and menopause. Krejci found female hormones that fluctuate throughout women’s lives can change conditions in the mouth that allow bacteria to grow, enter the blood, and exacerbate certain health issues like bone loss, fetal death and pre-term births.
Her overview of the literature was reported in the article, “Women’s Health: Periodontitis and its Relation to Hormonal Changes, Adverse Pregnancy Outcomes and Osteoporosis” in the May issue of Oral Health and Preventive Dentistry.
The Case Western Reserve University periodontist reviewed 61 journal articles with nearly 100 studies for a collective answer on whether hormones have a relationship to gum disease and specific women’s health issues like preterm labor, bone loss, and the side effect of hormonal replacement therapy.
“There’s definitely a gender-specific connection between women’s hormones, gum disease, and specific health issues impacting women,” Krejci said.
“Although women tend to take better care of their oral health than men, the main message is women need to be even more vigilant about maintaining healthy teeth and gums to prevent or lessen the severity of some of women-specific health issues,” Krejci said.
In addition to the brushing and flossing daily regimen, Krejci recommends visiting the dentist at least every six months, and more if there are any gum problems found or women suffer from bone loss or are pregnant.
She added that it is widely known that hormones cause some women gum problems during pregnancy. Women already susceptible to gum disease before being pregnant, she advises, need to make sure that these oral problems are treated.
Although women were once discouraged from seeing the dentist while pregnant, she said that scaling and planing of the roots of teeth to eliminate some gum disease is now recommended during pregnancy for women. Severe gum disease requiring surgery is still generally postponed until after the baby’s birth.
Gum disease begins with the build up of bacterial plaque on the teeth and under the gums. Untreated it can cause irritation and inflammation during which harmful and toxic byproducts are released. These toxins erode the bone that anchors teeth and cause breaks and bleeding in the gums.
Collaborating with Krejci on the study was Nabil Bissada, professor and chair of the Department of Periodontology at Case Western Reserve University School of Dental Medicine.
Source: Science Daily
Journal Reference:
- Krejci, Charlene B. / Bissada, Nabil F. Women’s Health: Periodontitis and its Relation to Hormonal Changes, Adverse Pregnancy Outcomes and Osteoporosis. Oral Health Prev Dent, 10 (2012), No. 1, Page 83-92 [link]
Do you really want to avoid cavities in your teeth and preserve a beautiful smile? Try massaging them with a high-fluoride toothpaste after lunch. “Rubbing toothpaste onto your teeth increases the fluoride protection by 400%,” says Anna Nordström, dentist, PhD and researcher at the Sahlgrenska Academy at the University of Gothenburg, Sweden.
Eight years ago a new brand of toothpaste was launched in Sweden with more than three times as much fluoride as standard toothpaste. Available without prescription, it is aimed primarily at those with high caries risk.
First scientific evaluation
Researchers at the University of Gothenburg’s Sahlgrenska Academy have now performed the first scientific evaluation of the effect of this so called “high-fluoride toothpaste.” The study has resulted in a new method that quadruples the level of protection from fluoride.
Four times better protection
In the study, 16 volunteers tested a variety of brushing techniques, using either high-fluoride or standard toothpaste, and brushing either two or three times a day.
“The study revealed that those who used a high-fluoride toothpaste three times a day had four times better fluoride protection in the mouth than those who used standard toothpaste twice a day,” says researcher Anna Nordström from the Institute of Odontology at the Sahlgrenska Academy.
Rub your teeth after lunch
Also tested was a new method developed in collaboration with professor Dowen Birkhed, which involves rubbing toothpaste onto your teeth with a finger.
“This ‘massage’ method proved to be at least as effective as a third brushing in increasing the amount of fluoride in the mouth,” Anna Nordström explains. “Rubbing the front of your teeth with toothpaste can be an easy way of giving your teeth a third “shot” of fluoride during the day, after lunch for example. But this should not replace brushing with a fluoride toothpaste morning and evening — it’s an extra.”
Daily use is essential
Brushing with fluoride toothpaste has played — and continues to play — a major role in combating tooth decay, and there is strong scientific evidence that daily use of fluoride toothpaste has a pronounced preventive effect.
The study Effect of a third application of toothpaste (1450 and 5000 ppm F), including a “massage” method, on fluoride retention and pH drop in plaque was published in Acta Odontologica Scandinavia.
THE RESEARCHER´S TOP TIPS • Use toothpaste at least twice a day, after breakfast and before going to bed. • If necessary, brush a third time or rub on some toothpaste instead. • If you have problems with cavities, choose a toothpaste with a higher fluoride content. • Avoid rinsing out the toothpaste with water.
SOURCE: Science Daily
Journal Reference:
- Anna Nordström, Dowen Birkhed. Effect of a third application of toothpastes (1450 and 5000 ppm F), including a ‘massage’ method on fluoride retention and pH drop in plaque. Acta Odontologica Scandinavica, 2012; : 1 DOI: 10.3109/00016357.2011.654238
A novel bacterium, thought to be a common inhabitant of the oral cavity, has the potential to cause serious disease if it enters the bloodstream, according to a study in the International Journal of Systematic and Evolutionary Microbiology. Its identification will allow scientists to work out how it causes disease and evaluate the risk that it poses.
The bacterium was identified by researchers at the Institute of Medical Microbiology of the University of Zurich and has been named Streptococcus tigurinus after the region of Zurich where it was first recognised. S. tigurinus was isolated from blood of patients suffering from endocarditis, meningitis and spondylodiscitis (inflammation of the spine). It bears a close resemblance to other Streptococcus strains that colonise the mouth. Bleeding gums represent a possible route of entry for oral bacteria into the bloodstream.
The similarity of S. tigurinus to other related bacteria has meant that it has existed up until now without being identified. Its recent identification is clinically important, explained Dr Andrea Zbinden who led the study. “Accurate identification of this bacterium is essential to be able to track its spread. Further research must now be done to understand the strategies S. tigurinus uses to successfully cause disease. This will allow infected patients to be treated quickly and with the right drug.”
Dr Zbinden said that while the discovery of the bacterium is no cause for alarm, it is important that it is recognised and the risk is quantified. “This bacterium seems to have a natural potential to cause severe disease and so it’s important that clinicians and microbiologists are aware of it,” she said. “The next step is to work out exactly how common this bacterium is in the oral cavity and what risk it poses. Immunosuppression, abnormal heart valves, dental surgeries or chronic diseases are common predisposing factors for blood infections by this group of bacteria. However, the specific risk factors for S. tigurinus remain to be determined.”
Photo: CCOS
Source: Science Daily
Journal Reference:
- A. Zbinden, N. J. Mueller, P. E. Tarr, C. Sproer, P. M. Keller, G. V. Bloemberg. Streptococcus tigurinus sp. nov., isolated from blood of patients with endocarditis, meningitis and spondylodiscitis. International Journal of Systematic and Evolutionary Microbiology, 2012; DOI: 10.1099/ijs.0.038299-0
Immediate placement of a dental implant right after a tooth is extracted, along with attachment of the temporary tooth, is a predictable treatment option for patients who must lose a tooth. My partner and I have been placing dental implants in our private periodontal practice in Newton and Framingham, MA for over 25 years. We have personally witnessed the evolution of implant dentistry to this point. Patients are thrilled with the results of “same day” dental implants and restoration. And, the esthetic results are typically outstanding; usually better than the outcomes that are achieved in delayed, staged-out treatment protocols.
Critical factors for success include using an implant that provides superior stability in the bone of the extraction socket, right after the damaged tooth has been removed. We also prefer using an implant that has a “platform shift” design to avoid loss of crestal bone during healing. An internal connection is also desirable to provide maximum stability for the abutment which supports the crown (tooth). The NobelBiocare NobelActive implant fixture has been the perfect solution for us.
Comments are welcome.
Gum disease affects millions of people around the work. And, gum recession ( the loss of gum tissue and supporting bone around a natural tooth) makes up a big part of the problem. Unfortunately, loss of gum and bone can eventually lead to tooth loss.
But there is a cure! Dentists and periodontists (dentists who specialize in the treatment of gum disease) can repair the damage caused by gum recession. With a traditional treatment approach, a small amount of gum can be removed from another part of the mouth and used to repair the tooth that has lost gum. The exposed root can oftentimes be covered to improve the cosmetic appearance of the tooth. This is generally considered to be the “gold standard” of treatment because the patient’s own gum is used. The downside is that the area that the gum is borrowed from (it grows back) can be sore during the healing phase after treatment.
Over the years, various materials have been developed to be used as a substitute for using the patient’s own gum as the donor. These include donor grafts from cadavers……Yes, it sounds unappealing, but it is perfectly acceptable and has been used for decades. Newer materials are now available that are made from collagen (the building block of all skin)! The general benefits include avoiding a second surgical site to borrow the gum, so there is less soreness. And the results appear to be quite promising.
We, at Periodontal Associates, have been using Mucograft collagen matrix for awhile now with much success in treating gum recession (and, no, we do not have any affiliation with the company). Our patients are very happy with the outcomes which include improved cosmetic appearance, improved gum health, and their improved quality of life.
Comments are appreciated!
My partner, Giovanni Castellucci, and I have been placing dental implants in our periodontal practice for over 27 years. Every day, we see an ever increasing amount of requests from our restorative colleagues and patients from Boston, Newton, Framingham, and the surrounding metrowest communities for extraction of a compromised tooth, followed by immediate dental implant placement and restoration (Teeth in a Day). Years ago, this was a very challenging proposition for a variety of reasons, and we oftentimes had to decline these requests and follow a more traditional treatment protocol. However, with the current advances in dental implant design (including surface technology, thread pattern, and restorative connection), we can confidently and predictably deliver immediate dental restorations in one dental appointment. One of our favorite dental implants for “teeth in one day” is the NobelActive fixture from NobelBiocare. We have been impressed by the tremendous stability at insertion (70 Ncm), platform switch – bone preservation design, surface technology to maximize bone-implant contact and osseointegration, and ease of restoration.
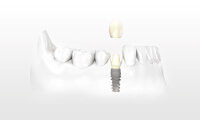 Case selection is paramount to assure a successful outcome, and not every patient is truly a candidate for these procedures. Every case has to be thoroughly evaluated on its own merits. And, there is no substitute for clinical experience and surgical expertise. In the end, our mission is to have a happy and healthy patient with normal function and a beautiful smile.
Case selection is paramount to assure a successful outcome, and not every patient is truly a candidate for these procedures. Every case has to be thoroughly evaluated on its own merits. And, there is no substitute for clinical experience and surgical expertise. In the end, our mission is to have a happy and healthy patient with normal function and a beautiful smile.
Have any of you had similar experiences? Please share them with the community.
Cary Feuerman, DMD
PERIODONTAL ASSOCIATES
photo credits:
Dental Implant #9 – Cary Feuerman, DMD
NobelActive Graphic:

Scientists are reporting identification of two substances in licorice — used extensively in Chinese traditional medicine — that kill the major bacteria responsible for tooth decay and gum disease, the leading causes of tooth loss in children and adults. In a study in ACS’ Journal of Natural Products, they say that these substances could have a role in treating and preventing tooth decay and gum disease.
Stefan Gafner and colleagues explain that the dried root of the licorice plant is a common treatment in Chinese traditional medicine, especially as a way to enhance the activity of other herbal ingredients or as a flavoring. Despite the popularity of licorice candy in the U.S., licorice root has been replaced in domestic candy with anise oil, which has a similar flavor. Traditional medical practitioners use dried licorice root to treat various ailments, such as respiratory and digestive problems, but few modern scientific studies address whether licorice really works. (Consumers should check with their health care provider before taking licorice root because it can have undesirable effects and interactions with prescription drugs.) To test whether the sweet root could combat the bacteria that cause gum disease and cavities, the researchers took a closer look at various substances in licorice.
They found that two of the licorice compounds, licoricidin and licorisoflavan A, were the most effective antibacterial substances. These substances killed two of the major bacteria responsible for dental cavities and two of the bacteria that promote gum disease. One of the compounds — licoricidin — also killed a third gum disease bacterium. The researchers say that these substances could treat or even prevent oral infections.
Source: Science Daily
Journal Reference:
- Stefan Gafner, Chantal Bergeron, Jacquelyn R. Villinski, Markus Godejohann, Pavel Kessler, John H. Cardellina, Daneel Ferreira, Karine Feghali, Daniel Grenier. Isoflavonoids and Coumarins fromGlycyrrhiza uralensis: Antibacterial Activity against Oral Pathogens and Conversion of Isoflavans into Isoflavan-Quinones during Purification. Journal of Natural Products, 2011; 74 (12): 2514 DOI: 10.1021/np2004775